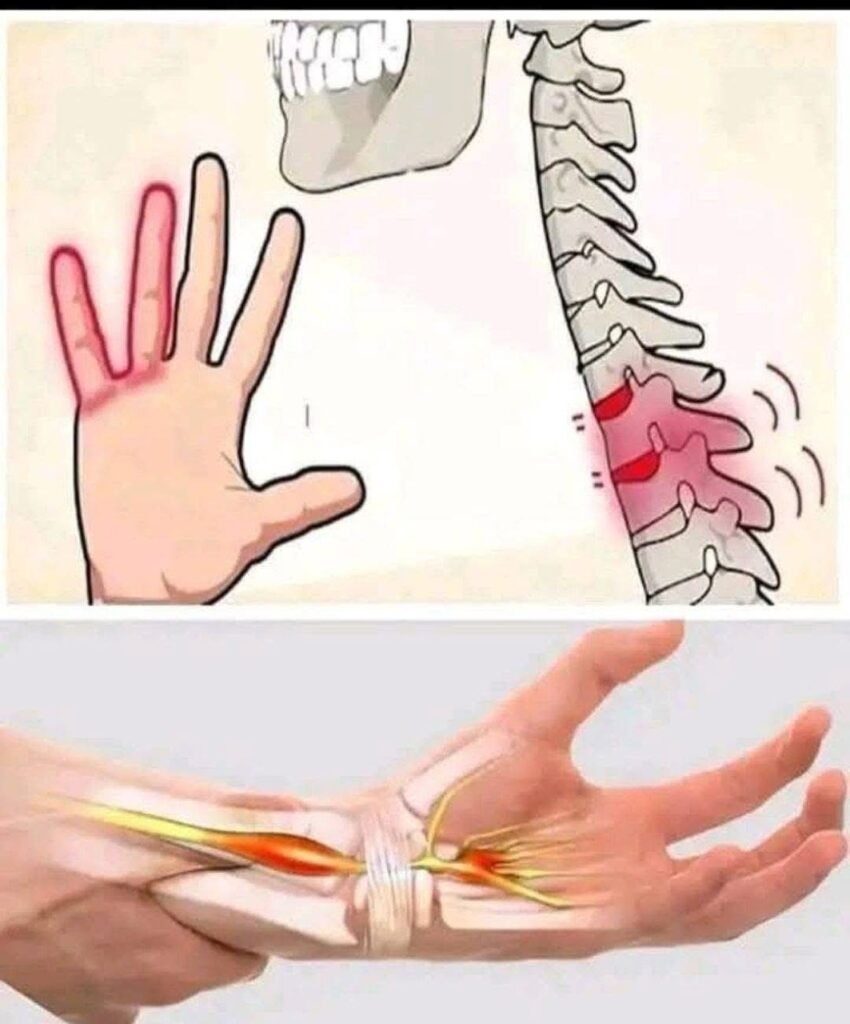
Paresthesia is the medical term for the sensation of tingling, prickling, numbness, “pins and needles,” or skin crawling — without a clear physical cause (like an insect).
It happens when there is pressure, irritation, or damage to a nerve, or disruption in the signal between the nerve and the brain.
🔹 Common Examples (Most People Experience These)
| Type | What it feels like | Why it happens |
|---|---|---|
| Temporary paresthesia | Limb “falls asleep” | Sustained pressure cuts off blood flow / nerve compression (sitting on foot, sleeping on arm) |
| “Hit your funny bone” | Sharp electric tingle in elbow/forearm | Ulnar nerve compressed against humerus bone |
| Waking up with numb hand | Tingling, weak grip | Wrist bent during sleep compresses median or ulnar nerve |
✅ Temporary paresthesia resolves within minutes of moving, shaking, or changing position.
🔹 Chronic / Persistent Paresthesia
If tingling is recurrent, persistent, or has no obvious trigger, it may point to an underlying condition.
Common causes:
-
Nerve entrapment / compression
-
Carpal tunnel syndrome (thumb, index, middle finger)
-
Cubital tunnel syndrome (ring & pinky finger)
-
Sciatica (tingling down leg)
-
-
Peripheral neuropathy
-
Diabetes (most common)
-
Alcohol use disorder
-
Vitamin B12 deficiency
-
Chemotherapy side effect
-
Hypothyroidism
-
-
Circulatory issues
-
Raynaud’s phenomenon (fingers turn white/blue, tingle upon rewarming)
-
Peripheral artery disease (less common)
-
-
Neurological conditions
-
Multiple sclerosis (often one side, comes and goes)
-
Stroke or TIA (sudden onset, one side of body)
-
Migraine with aura
-
-
Anxiety / panic attacks
-
Tingling around mouth, hands, feet — often from hyperventilation
-
-
Autoimmune / inflammatory
-
Lupus, rheumatoid arthritis
-
Guillain‑Barré syndrome (rapid ascending weakness + tingling — emergency)
-
🔹 When to See a Doctor
Seek medical attention if:
-
Tingling follows head injury, fall, or trauma
-
It’s sudden, one‑sided, and accompanied by weakness, confusion, drooping face, or trouble speaking — call 911 (possible stroke)
-
It spreads rapidly up a limb
-
Loss of bladder or bowel control
-
You have a known condition (diabetes, autoimmune disease) and symptoms are new or worsening
-
Tingling is persistent and interferes with sleep or daily tasks
🔹 What Helps (Depends on Cause)
| Cause | Approach |
|---|---|
| Temporary compression | Move, massage, stretch |
| Carpal tunnel | Wrist splint at night, ergonomic changes, PT |
| B12 deficiency | Supplement (oral or injection) |
| Diabetic neuropathy | Blood sugar control, specific meds (gabapentin, duloxetine) |
| Pinched nerve in spine | Physical therapy, anti‑inflammatories, sometimes surgery |
| Anxiety‑related tingling | Breathing exercises, stress management |
🔹 Paresthesia ≠ Always Bad
-
Goosebumps = piloerection — sympathetic nervous system, not technically paresthesia but similar “skin sensation”
-
ASMR or emotional chills — tingling scalp/spine — also not pathologic
🧠 Bottom Line
Temporary paresthesia is harmless.
Chronic or unexplained tingling is a symptom — not a diagnosis — and deserves a workup.
Start with your primary care doctor. They’ll check:
-
Basic blood work (CBC, B12, thyroid, glucose)
-
Physical/neurological exam
-
Possibly refer to neurology for EMG / nerve conduction studies
Would you like a breakdown of tests doctors use to diagnose the cause of paresthesia?